My body is exhausted but my mind won’t let me sleep. The films of last week’s events are on a repeat-loop in my head, so let me share some of it with you. Let’s watch the blockbuster of Carol’s death in hospital, exactly a week ago today. It’s just over two hours long, from my arrival in hospital to the moment she died.
I’m happy and grateful that I could be an actor in that film, but as befits a grieving person, I’m also troubled by what-if’s and if-only’s. What if the script could have been changed a bit here, a bit there? If only.
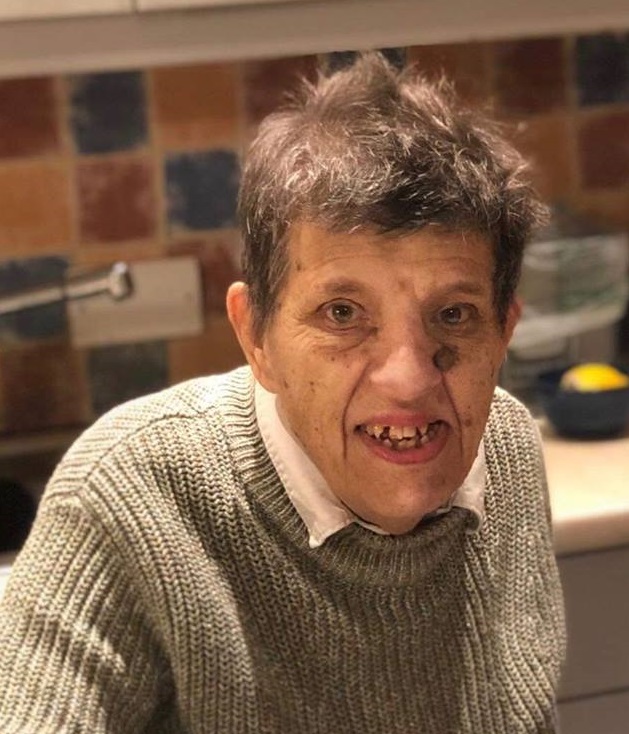
Carol
Carol was 68 years old.
She was a force of nature, fighting off infections and other episodes of unwell-ness over the past years. The assistants (as we call the “support staff” who spend her days with her, some of whom live in her home) were attentive to her medical needs, so when she complained about her legs and she seemed to have lost strength in them, they were alarmed and took her to hospital.
She spent the night in A&E. Hazel telephoned me the following morning, still in A&E. She had been with Carol since midnight. All that time, Carol had been desperate and unable to get comfortable, grabbing onto Hazel, moaning, trying to shift position. The doctors had diagnosed a very large clot in the main blood vessel in her abdomen, supplying the lower part of her body. Her right leg was already stone cold.
She finally fell asleep in Hazel’s arms around 7.30, probably from sheer exhaustion. Two hours later, five doctors came past and said,
“We can’t operate. It’s palliative care only from now on.”
And left.
At least I think that is the story I heard from Hazel. She phoned me and burst into tears. Phone reception in A&E (and, as we would later discover, on the ward) is poor, so she kept cutting out and I couldn’t quite work out what was happening. Blood clot? Palliative care? What does that mean? Some people receive palliative care for months, years even. Is Carol dying? Or is she simply needing quality-of-life-care that could last a long time?
I had no idea, and as far as I could make out from the dodgy phone line, neither could Hazel, who anyway needed to be with Carol in her state of in-and-out-sleep. Who to ask? Doctors and nurses were running around the busy A&E department, saving lives and limbs of other patients. But Hazel’s distress was concern enough. She is one of the most experienced assistants in the L’Arche community, she’s been around for decades, she is a mature woman who has seen a lot of life and of death. Help was clearly needed.
“I’m coming,” I said to Hazel, who cried some more at that. “I’ll be there in an hour.”
I changed from my jeans and jumper into my power jacket. Sometimes it’s easier to get answers from doctors and nurses if you look like someone in authority, and I’ve got a fancy new title of Professor Of Palliative Care And Learning Disability, so that might help (it shouldn’t, but I find that it does). Better look the part, so they’ll believe me.
By the time I got to the hospital, Carol had finally been found a bed on the ward, in a side room. She looked at me, recognised me, grabbed hold of me, grabbed hold of the bedside, trying to shift position. “She’s been like this all night,” Hazel despaired. “In fact it’s much better now, it was far worse.”
Hazel knows about people dying. I looked at Carol and I looked at Hazel.
“This doesn’t look good,” we agreed. “She may be in her final days.”
Someone who needs “palliative care” can live for a long time – that’s not the same as dying. What I mean by “dying” is the point of no return, when the body starts shutting down, and there is nothing anyone can do to stop it or even to slow it. No need (indeed no point) to try and feed the person, or give them a drip, because it won’t make them live any longer. Dying is a natural process that can last a few minutes (as it did for Michelle) or, at a push, a few weeks (as it did for my mother, who found dying difficult and was hanging on and on), but usually it’s somewhere between a couple of hours and a couple of days.
Doctors and nurses (especially hospice nurses like myself) learn to recognise this phase. Breathing changes. People may slip into unconsciousness, then wake up again, then slip away again for a bit longer. Sometimes they become restless – in my hospice days, we called it “terminal restlessness”.
I thought Carol’s occasional drifting-off-to-a-brief-sleep was in fact not sleep but a few moments of unconsciousness, and her agitation could well indicate that she was, in fact, dying. If I’d been her nurse, this is when I would call her family and tell them to come. Plus, I’d give her a bit of morphine and perhaps some midazolam (a sedative) as she was clearly in distress.
But I was not her nurse and I don’t know anything about your prognosis if you have a blood clot. Perhaps this was something people recover from, even if just for a while? I needed to find out.
I found Carol’s very lovely nurse and we looked at her drug chart together. She’d had morphine twice during the night. Please give her some more, I said. She needs it, and she needs it now. The nurse agreed but couldn’t, because morphine was only written up as an intravenous injection, which she wasn’t allowed to give. She needed to wait for a doctor to authorise it in a different format.
“She’s been referred to the palliative care team,” said the nurse. “The doctor is coming soon.”
Now, that’s wonderful, but how soon is soon? If you only have two hours to live (which is what it turned out to be), then an hour’s wait is half a lifetime.
Next, the surgeon came onto the ward, thank goodness. He was the doctor who saw Carol in A&E last night. He called me out of the side room and explained about the blood clot and his inability to operate. He was touched by Carol’s personality, by her story (I gave him the headlines), and said, “She’s not going to survive this.”
She’s not going to survive this? Translation, please? What exactly does this mean?
I needed him to be absolutely clear, so I asked him.
“Does this mean that she is going to die in this room, and that it is going to happen soon? Is she dying now? Are we talking about a few days, at most?”
Yes, he said. Yes. That’s what it means.
“Thank you,” I said. Because we needed to know this. Hazel hadn’t known it, because nobody had spelled it out.
“Can she stay here?” I asked both him and the lovely nurse. She could.
“In that case,” I said, “I hope it’s OK if we take over that room. Carol has a lot of friends, and they will want to come and see her. Be prepared for an invasion.”
Here is the if-only.
If only the doctors had told us immediately that “we can’t operate” means “she is dying”. Presumably, they knew this last night. There is no way Carol’s carers could have known, or would even have known to ask. But if doctors know that Carol had already reached the point of no return, then why didn’t she have the right end-of-life drugs immediately, to make sure her dying was more comfortable? And why, come to think of it, wasn’t there an immediate discussion of where this dying was going to happen? We might have brought her home.
But at least now we knew. Two more assistants had already arrived at the same time as myself, and between us we wandered around the corridors trying to find the best phone signal, and put word out. It spread like wildfire. Carol does, indeed, have very many friends, and they did start to arrive.
First to make a brief visit was Carol’s housemate Serena with two more assistants. I was impressed they managed to bring Serena in so quickly – it was important, because Serena doesn’t understand words, so there was no other way to explain what was happening with Carol.
We also called the priests from Carol’s church, and one of them came quickly, calm and reassuring.
The other person who turned up was the palliative care consultant. I could have kissed her. (In fact I did, because I knew her from my hospice days and hadn’t seen her for years, and she’s brilliant.) She wrote up the morphine and midazolam Carol needed. I asked her to spell things out again. She is dying, yes? We’re talking hours to days?
“Yes. I’m thinking days,” said the consultant. I looked at Carol, who, even before those long-awaited injections of morphine and midazolam, had relaxed into what seemed like sleep but what was really unconsciousness. I looked at Hazel. Hm, I thought. I’m thinking hours. But the consultant thought we might have enough time to consider getting Carol home, if that’s what we wanted.
We talked about this and we agreed that yes, that would be good. I explained to everyone (by now, there were around eight of us sitting around the bed) about the unconsciousness. We thought that for Carol it would be fine to die here, comfortable now, with her friends around her.
But for everyone else, it would be so much better if Carol died at home.
Then everyone could take time to sit with her, both before and after she died.
So that was the plan. Bring Carol home. Tomorrow morning perhaps, the consultant had suggested.
My power jacket lay discarded in a corner. In the face of death, we are powerless, and we all have power. We lowered the bed and took down the bedsides, which were like barriers. We sat with her – priest on one side, me holding Carol’s hand on the other side. The priest prayed, putting her face close to Carol’s, and we think Carol knew, even though she was very deaf and wouldn’t be able to hear us talking. We sang The Lord is my shepherd. And I could see Carol’s breathing change. She was taking the slow, intermittent, deep breaths of someone very close to death. There was a profound intensity in the room, and a strong sense of togetherness.
It seemed entirely appropriate that just at that moment, Manuela (who also shares Carol’s home) came into the room with two young assistants. Like Serena, she needs explanation-through-experience because she doesn’t understand words. Carol loved Manuela, and she liked new people – she’d always welcome newcomers before anyone else did, with open arms (and a sloppy kiss). Helloooo! What’s your name?
The priest had reached the end of her prayer.
“Carol is taking her last breaths,” I said quietly to the new arrivals, who looked somewhat alarmed at the gasps and the gaps between the gasps. “It’s OK. This is normal, she is comfortable. She will just take another breath in a moment, and perhaps another one… It is OK.”
The priest ended the prayer.
And in the silence that followed, Carol died.
It was OK.
Carol’s dying had become a community event.
She was surrounded by the people from her community, old friends like myself and Manuela, new friends like the young assistants. We sat and sat. We were moved. We felt privileged. When someone dies, the world goes quiet. Even Manuela, who likes to make a lot of noise – especially when there are people around, especially in new environments – was quiet.
And we stayed for hours. We asked the nurse if that was OK, and it was. More people came. We washed Carol gently. Even in death, she brought people together – there we were, these young new friends who were in tears, and her old friends who were also in tears. A community of women who will carry this experience with them and pass it on, and be less afraid of death now.
Because Carol showed us that in the end, there is no need to be afraid.

Pingback: Helping people with profound intellectual disabilities cope with bereavement |
I love your writing so a lot! percentage we keep in touch extra about your post on AOL? I need a specialist on this house to unravel my problem. Maybe that is you! Looking ahead to look you.